Many people have heard of a procedure called “dry needling” but are not familiar with trigger point injections, which are used to treat what most people believe is “TMJ,” when the pain is actually caused by muscles. Trigger point injections and dry needling are the same procedure with one major difference. Trigger point injections involve the use of 1% plain lidocaine to numb the area being treated, which makes the procedure more comfortable whereas nothing is injected with dry needling. The use of lidocaine provides immediate feedback that the diagnosis is truly muscular in origin. If the trigger point injection reduces or eliminates the pain, then the source of the pain is the local muscle that was injected. However, it is not the lidocaine that provides the long-term relief. It is the needling that is done. Needling involves poking the local muscle with a very thin needle for 30 to 60 seconds, which intentionally induces inflammation into the area, which the body will repair in 24-48 hours. This is not a painful procedure as it is more of a sensation but it is common to be sore for a day or two after the procedure.
The protocol we follow in our practice is to try trigger point injections first and see what type of relief is provided. The relief can range from “one and done,” meaning the pain does not return. If there is a benefit but it is only one week, then I repeat the procedure again. The second round can set the pain free, last a few months or again last as short as a week. If the pain is relieved but only for about a week, then Botox can be used for long term relief. The benefit from the Botox also varies from setting the pain free to lasting two to three months. Some patients get a longer relief with the second round of Botox and some need Botox every three months.
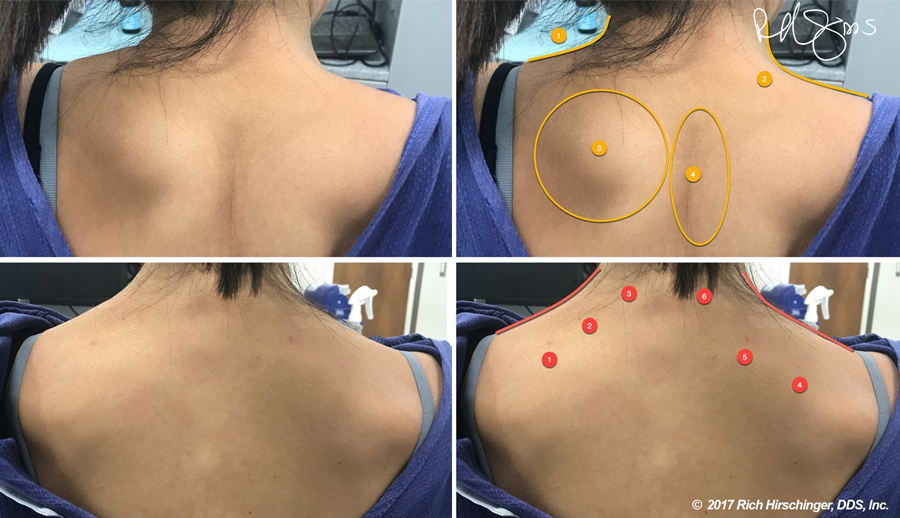
It is difficult to “see” the benefit of trigger point injections with facial muscles but the benefit from the treatment we provided (during residency training) below to one of our patients is clearly visible. She presented with a very stiff neck and she could not move her head very much from side to side. The trapezius (shoulder) and splenius capitis (back of neck) muscles were in severe contraction, which you can see in the top row with the upper right outlining the contraction areas. I did trigger point injections using 1 cc 1% lidocaine into several locations. You can see the injection sites for the trapezius, which are identified with the red numbers on the bottom right. Notice the relaxed lines of the trapezius in the red lines in the bottom right. She had full mobility after these injections.
What is a trigger point?
A myofascial trigger point, or knot, is a hyperirritable spot, usually located within a taut band of skeletal muscle, which feels painful upon compression and can give rise to characteristic pain, motor dysfunction, and autonomic phenomena. Trigger points produce local and referred pain and often accompany chronic musculoskeletal disorders.
Knots can be felt as nodules or bands in the muscle. Stimulation of a knot may elicit a twitch response and pain, which may radiate in a distribution consistent with the affected muscle. A trigger point may produce not only pain in the affected muscle, but in a distant area, including locations in the head and neck, called referred pain. Trigger points may develop because of trauma, injury, inflammation, or other factors.

What is a trigger point injection?
A trigger point injection can help soothe muscle pain, especially in your shoulders, neck and facial muscles. It also can be used to treat tension-type headaches, cervicogenic headaches, TMJ pain and myofascial pain. Trigger points are painful “knots” in your muscles. They form when a muscle can’t relax. Sometimes you can feel these knots when you rub your muscle.Injecting small amounts of anesthetic along with “needling” into the trigger point can help alleviate the pain.
Who should receive trigger point injections?
Patients that have specific trigger points that can be elicited with palpation (a firm touch) may experience the most relief from injections. They may be very helpful for immediate relief for severe pain in patients with an individual headache or migraine attack, or can help treat an overall worsening of head pain in patients with chronic headache disorders who are having an exacerbation.


How do trigger point injections performed?
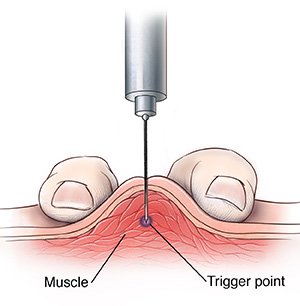
In the trigger point procedure, a health care provider inserts a small needle into the patient’s specific area of pain (trigger point) in a muscle. The injection usually contains only a local anesthetic. This procedure can be performed in a doctor’s office, and does not require sedation. The patient is positioned sitting or lying down. Your doctor will first palpate and identify the painful areas within a muscle. After identifying such trigger points, your doctor will inject those areas. Depending on how many trigger points are identified, more than one injection may be required. Imaging is not needed to diagnose a trigger point as they do not show up on x-rays or MRIs. However, if an underlying condition is the cause of the trigger point, then these tests can be helpful. You can have several trigger points injected during one visit to your doctor’s office. The procedure only takes a few minutes.
How do trigger point injections work?
The anesthetic medication will be injected into the muscle and will block pain receptors within the nerves surrounding the muscle, and, in turn, reduce the pain signals sent to the brain. If steroid medication is used, it reduces the inflammation and swelling of tissue around the nerves, which may help reduce pain. The needle without medication may even provide independent benefits mechanically. The needle separates, relaxes and lengthens the muscle fiber to provide further pain relief. This approach is called “needling” and may be used in patients with allergies to anesthetic medication.
Are trigger point injections safe?
The risk of complication from a trigger point injection is very low. Complications such as bleeding and infection at the injection site are uncommon. However, you may have temporary soreness or numbness at the injection site.The most common side effects are temporary pain and numbness at the injection site. Infection and bleeding may occur at the injection site, but this can be avoided by cleaning the site before injection and applying pressure to the site after injection.
What can I expect after receiving trigger point injections?
Immediately after the injection, you may feel that your pain has remitted or lessened significantly, in both the affected muscle as well as the area of the referred pain in the head or neck. Some patients may not benefit at all, while others may have significant pain remission lasting for weeks. You can return to your daily activities immediately after the injections. Health care providers may repeat the procedure as needed and customize how often it is performed.
Post-procedure care?
To ensure the best success with trigger point injections, post-procedural care may include the following.
1. Proper Stretching
While it’s important not to overstress the muscle, it is still recommended that you use your muscles to their full range of motion to help relieve stiffness and reclaim normal muscle functioning. To help your muscles relax and optimize the effects of the injections, stretching after your trigger point injections is an integral post-procedure component. Your doctor will most likely stretch you as soon as the procedure is complete, and then send you home with instructions to continue proper stretching on your own.
2. Active Exercise
The whole purpose of undergoing trigger point injections is to restore full use of your muscles, and active exercise will help determine whether or not the treatment was effective. These exercises will target muscle stretching, muscle strengthening, and muscle conditioning to help relieve myofascial pain. Staying active with exercise will also help reduce the chances of developing more trigger points in your muscle fibers as you increase your muscle endurance.
References
- Travell JG, S.D., Simons LS, Travell and Simons’ Myofacial pain and dysfunction: The trigger point manual. 2 ed. Vol. 1. 1999, Baltimore MD: Williams and Wilkens.
- Graff-Radford SB. Myofascial pain: diagnosis and management. Curr Pain Headache Rep. 2004;8:463-467.